The importance of tummy time play cannot be overstated. Since the introduction of “Back to Sleep” in 1994, many published studies have cited an increase in medical diagnoses such as plagiocephaly, brachycephaly and torticollis*(see below for descriptions) and developmental delay of gross motor milestones. Though this program successfully cut in half the rate of Sudden Infant Death Syndrome (SIDS), the rise of other mostly-preventable diagnoses illustrate some of the unintended consequences of “Back to Sleep.”
Many parents are anxious or even fearful about the tummy down position because of its connection to SIDS. Just because an infant is awake, that anxiety does not dissipate, so parents often avoid placing their infants on their tummies from the start. In addition, parents are not aware of the importance of tummy time when babies are awake, so there is little reason for them to even try.
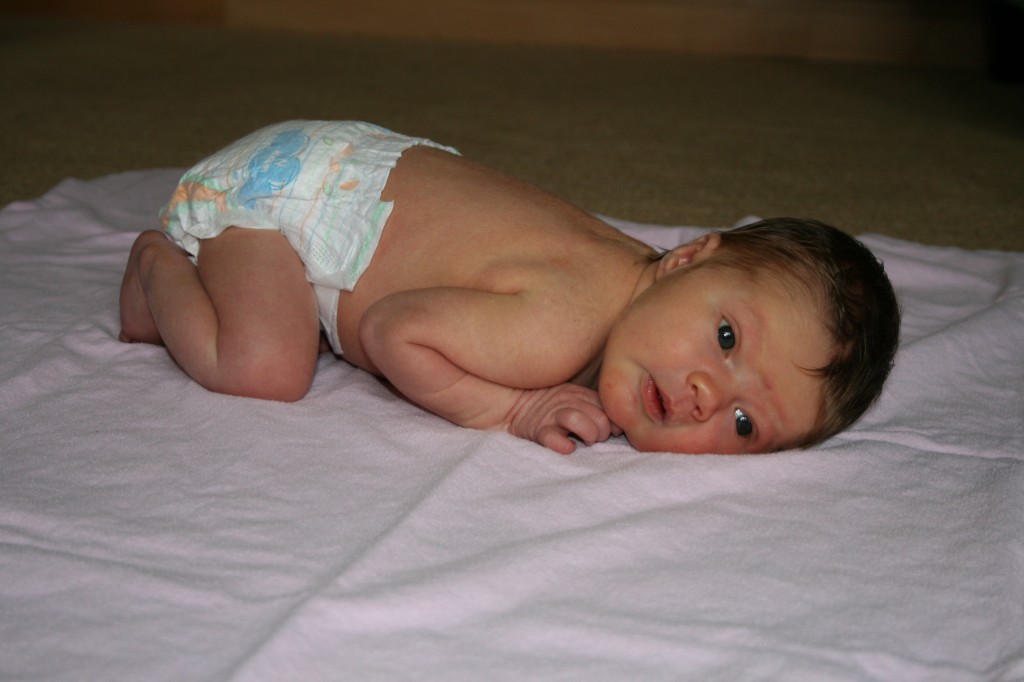
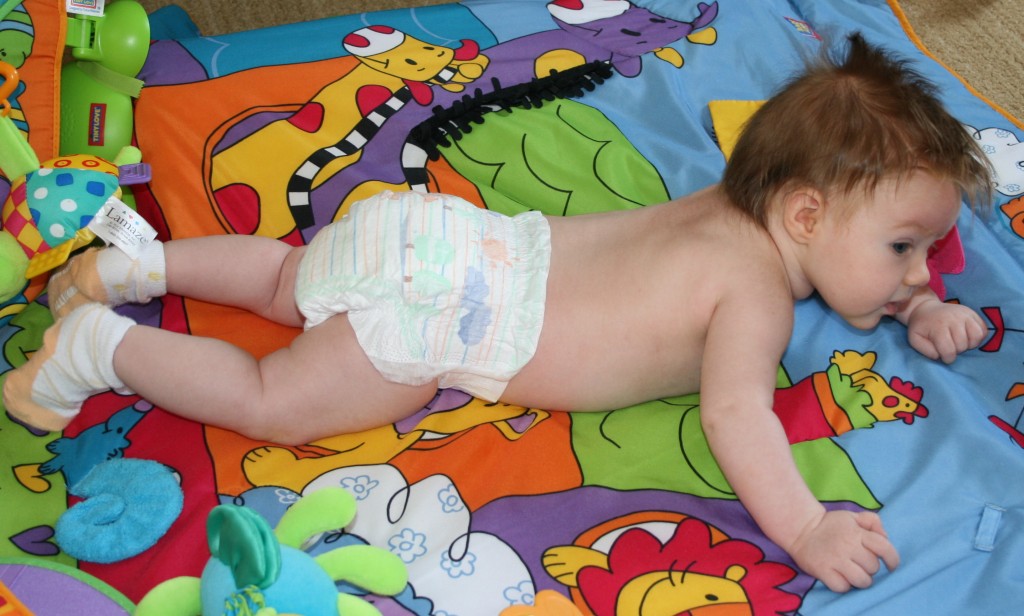
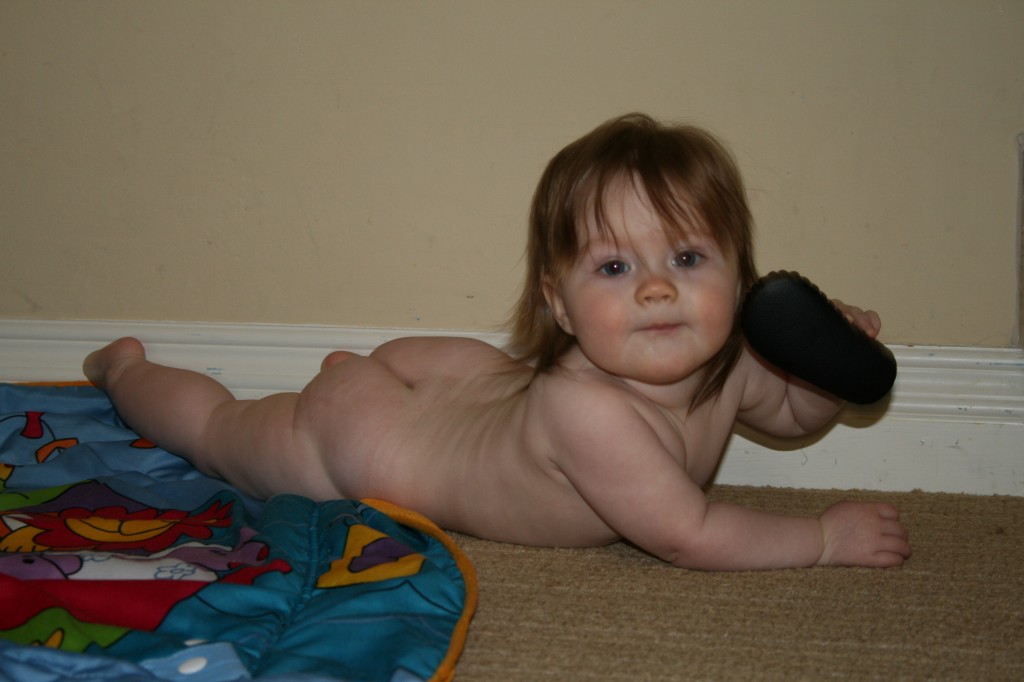
Tummy time is important for many reasons. Babies are often positioned in utero in asymmetrical positions, and many stay in the same position for most of pregnancy. These asymmetries do not disappear overnight after babies are born. They need to be worked out with babies’ spontaneous movements against the floor and gravity. Babies need to have plenty of time to move freely on the floor, to be out of containers such as car seats, infant seats, swings, and strollers. The position of choice when putting an awake baby down should be tummy down. Newborn babies do not have the strength to lift their heads for sustained periods of time. They rest their head on the floor with their cheek in contact and their neck turned 90 degrees. As long as they position themselves looking both directions, gravity and the floor provide a long, low-load stretch on the SCM and other muscles implicated in torticollis. Tummy time also eliminates any pressure on the back of the head, preventing flatness or allowing any flat spots to round out.
Parents should look at their baby from head to toe after birth to look for any asymmetries in baby’s preference for turning his head or flexing his body one direction or another. Parents can also take pictures of head shape over time to ensure that any flat spots round out. Keeping a photo diary or a log of activity over time helps parents to determine patterns that either exacerbate or alleviate any asymmetries present at birth.
I looked at a few different smart phone applications that would help me do just this after my son was born. I settled on iBabyLog, which is a great tool to track nursing, diapering, sleeping, and activity schedules (many other categories are also available for tracking). I can customize my comments, take photos, and easily look at patterns over time to track progress. For example, when putting my newborn son down for sleep, I make sure that he looks to the left one time and then to the right the other. When working on awake tummy time, I also track the time he looks left versus right. With the ability to track and summarize positions and alignment over the day and the week, it is easy for parents to notice any asymmetries that are present. And, at this very young age, parents have the power to fix asymmetries early with great results.
Using iBabyLog or other tracking tools to document positions during sleep and awake times can help parents to be more aware of their baby’s alignment. Proper alignment is a crucial foundation to symmetrical movement, which is essential for baby to properly achieve motor milestones. By being aware and tracking some of the foundation elements of movement, parents can intervene early and prevent medical problems in alignment and movement from ever occurring.
* Plagiocephaly is a misshapen head secondary to abnormal and asymmetrical forces placed upon the skull as an infant’s head is growing. It causes a diagonal asymmetry with flatness on the back of one side of the head and protrusion of the opposite forward side. It affects the shape of face, position of eyes and ears, and shape and symmetry of joints of the jaw and cervical spine. Since “Back to Sleep” began, the incidence of plagiocephaly has increased from 1 in 300 to 1 in 15. Though many pediatricians state that misshapen heads are merely a cosmetic issue, there are two very important joints that articulate with and are affected by skull shape: the jaw (TMJ) and the upper cervical vertebrae (OA). Atypical alignment in any joint, but especially those that require simultaneous action of two sides, increases abnormal wear and tear, leading to premature joint breakdown, arthritis and pain. Though this is a well-known and accepted medical phenomenon, because the first “Back to Sleep” babies are only 18 years old, long-term consequences of this specific malalignment due to misshapen heads have not yet been documented in medical literature.
* Torticollis is a shortening of the sternocleidomastoid (SCM) muscle on one side of the neck. Other neck muscles can be involved as well, but this muscle is most often implicated because of its long ropelike and very superficial location. When this muscle is short/contracted, your baby will have a head tilt to the same side, rotate to the opposite side, and prefer to extend head backwards rather than tuck his chin. Babies often avoid turning their head in the other direction and cannot achieve midline orientation of the head. Torticollis can be congenital, most often due to position in utero, or acquired, often due to asymmetrical head shape and positioning, such as with plagiocephaly. These two diagnoses frequently present together.
* Brachycephaly is a flatness on the back of the head that is more symmetrical from left to right, but causes protrusions laterally on both sides, making the face and head wider than otherwise would be. It reduces the space for the cerebellum to grow and decreases the distance between the back of the head and spinal cord, possibly placing the spinal cord at greater risk for injury with any head injury. It also changes the orientation of jaw and cervical spine joints. Brachycephaly is due to constant pressure on the back of the head from sleeping and positioning in infant “containers” such as car seats, infant seats, strollers, and swings.